The most common type of infectious esophagitis is Esophageal Candidiasis. The esophagus is the second most vulnerable to Candida infection in the gastrointestinal tract, after only the oropharynx. The fungus Candida causes esophageal thrush, an inflammatory condition of the esophagus. This is one of the most common digestive tract diseases, and it is the source of digestive disorders in the body. In this article, Illume will give you more details about Esophageal Candidiasis.

About Esophageal Candidiasis
The term “esophageal thrush” refers to a yeast infection of the esophagus. Esophageal Candidiasis is another name for this disease. Candida fungi are the cause of esophageal thrush. There are around 20 Candida species that can cause the disease, but Candida albicans is the most common.
Patients infected with the human immunodeficiency virus are more likely to develop Esophageal Candidiasis. This is due to the fact that around 10–15 % of HIV-infected people will acquire Esophageal Candidiasis over their lifetime, whereas the remaining 85–90 % will develop oropharyngeal candidiasis. Among a single-center study, we discovered that the incidence of Esophageal Candidiasis was 0.32 % in persons with high immunity in Korea.
Causes of Esophageal Candidiasis
The Candida fungus, which lives in the esophagus, is the most common cause of esophageal fungal infections. Candida is a parasitic fungus that lives in the human body, particularly in the esophagus, genitals, and skin… Candida fungus lives in harmony with other bacteria in a healthy human body, creating a balance of good and harmful bacteria.
When the host’s defense mechanism (such as the immune system) is weakened, Candida thrives in the esophagus mucosa and forms white sticky plaques. These plaques can be seen throughout the esophagus, as well as in the throat and mouth.
Symptoms of Esophageal Candidiasis
The symptoms of esophageal fungus are usually nonspecific, making it easy for the patient to mistake them with those of other gastrointestinal illnesses. The following are the most frequent symptoms of esophageal thrush:
- White lesions on the lining of your esophagus that look similar to cottage cheese and bleed if scraped
- Discomfort or pain when swallowing food
- Dry mouth
- Constant choking sensation
- Discomfort behind the sternum when swallowing.
- Other symptoms: abdominal pain, heartburn, weight loss, diarrhea, nausea.
Oral thrush can be observed on examination of the mouth; lesions may be isolated or combined in white patches on the mucous membranes of the mouth and pharynx, in the mouth, and on the tongue.
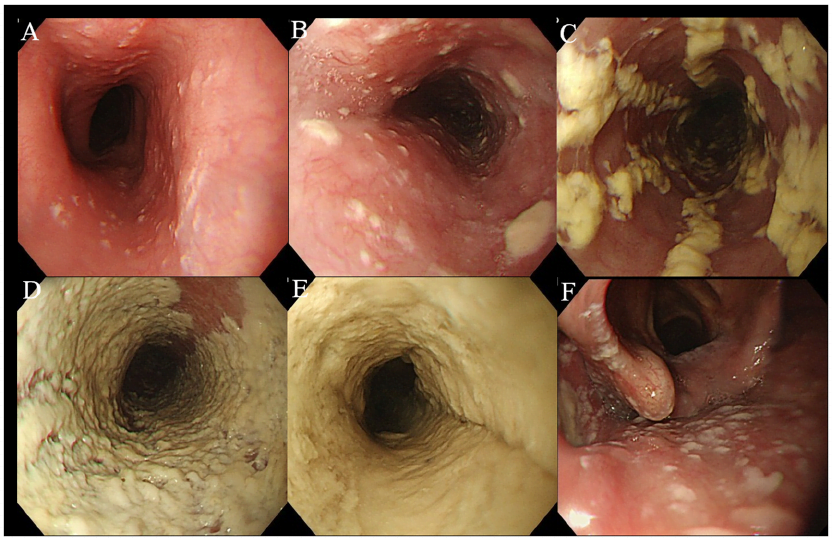
- A: Grade I, with many white swollen patches approximately 2 mm in size and no edema or ulceration.
- B: Grade II, many white swollen patches larger than 2 mm in size, no ulceration.
- C: Advanced level III array, starting to develop nodular arrays.
- D: grade IV, grade III results with greater mucosal friability and sporadic luminal stenosis.
- E: The appearance of a “white carpet,” a thick white plaque coating the lining of the esophagus and narrowing the lumen.
- F: Oral thrush, in which endoscopy can reveal laryngeal candidiasis.
Who is most prone to Esophageal Candidiasis?
In healthy individuals, esophageal mycosis is rare. The majority of people who have a Candida infection in their esophagus have weaker immune systems, which means their bodies don’t fight infections efficiently. Candida in the mouth and throat is common in people with Esophageal Candidiasis.
People at high risk of Esophageal Candidiasis:
- People infected with HIV/AIDS
- Diabetics
- People with immunocompromised system: cancer patients must undergo radiation, chemotherapy, long-term antibiotics, or corticosteroids.
- Individuals who smoke cigarettes regularly.
Diagnostics and testing
Doctors typically use esophagoscopy to diagnose the disease. Endoscopy is a technique for assessing the gastrointestinal tract that involves inserting a tube with a light and camera and directly observing white mucosal plaque lesions and mucous secretions.
How to treat Esophageal Candidiasis?
The treatment of esophageal thrush aims to eliminate the fungus while also preventing it from spreading.
Antifungal medicines are often used to treat Esophageal Candidiasis caused by Candida. Fluconazole, clotrimazole, miconazole, or nystatin are typical antifungal medicines. Different medicines are provided depending on whether the patient has a mild or severe fungal infection.
Late-stage HIV patients may require a more potent drug, such as amphotericin B. Most notably, treating HIV is essential for controlling Esophageal Candidiasis.
If your Esophageal Candidiasis has made it difficult for you to eat, your doctor may advise you on nutritional supplements. This can include high-protein drinks, if tolerated, or other feeding alternatives, such as a gastric tube in severe cases.
How to prevent Esophageal Candidiasis?
You can lower your risk of developing Esophageal Candidiasis by doing the following:
- Eating yogurt when taking antibiotics
- Maintaining proper dental hygiene.
- Visiting your dentist regularly for checkups.
- Limiting your intake of sugary foods.
- Reducing your consumption of yeast-containing foods.
Despite the fact that people with HIV and AIDS are at a higher risk for Esophageal Candidiasis, doctors seldom give antifungal medicines to prevent it. The yeast might develop resistance to treatments. If you have HIV or AIDS, you can minimize your risk of esophageal thrush by taking antiretroviral therapy (ART) medications as prescribed.

