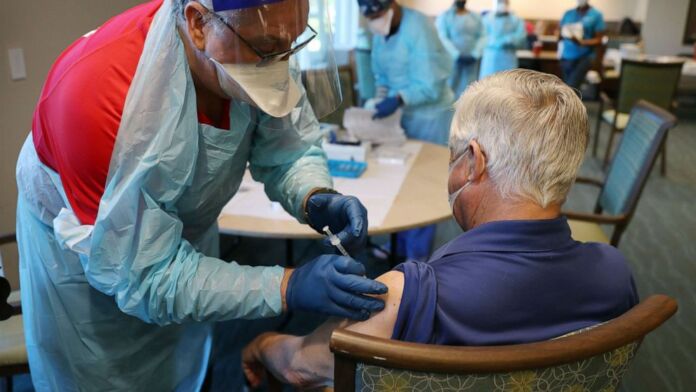
Labor shortages throughout the country are creating a race to retain and employ personnel as long-term care institutions deal with the delta variation.
With job openings in the United States reaching a record 9.2 million, nursing homes and other long-term care facilities are losing staff to other industries or to other nursing facilities that can offer higher wages and better benefits, according to long-term care advocates and health care associations.

Nursing home staff shortages are not new. However, advocates claim that the coronavirus epidemic, a general labor shortage, and an impending vaccination mandate for many long-term care institutions are making retention even more difficult.
As a result, several institutions have boosted their compensation, which has increased competition.
“There are places that give starting rates of $19 or $20 with massive sign-up incentives in the hundreds of dollars,” said Paul Liistro, CEO of Connecticut’s Manchester Manor and Vernon Manor nursing facilities. In comparison, Liistro said, his facilities are on schedule to pay licensed nursing assistants a $20 hourly rate within three years.
According to the US Bureau of Labor Statistics, the median annual pay for long-term care nursing aides – the majority of whom work full-time – was $30,120 in May 2020.
According to Liistro, several nursing facilities were able to increase staff wages temporarily during the pandemic’s early stages after receiving federal and state coronavirus relief money. However, Liistro stated that without that assistance, his facilities are unable to compete with the pay given in other locations.
And Liistro anticipates several resignations as a result of the forthcoming rule requiring his workers to either get vaccinated or undergo frequent testing.
The Biden administration stated on Wednesday that it will require nursing facility workers to be vaccinated against COVID-19 as a condition of obtaining federal Medicare and Medicaid funds. The White House’s new plan has already drawn criticism from activists who argue that it would further exacerbate personnel shortages.
“By focusing exclusively on nursing homes, we will drive vaccine-averse workers away from other health care providers, leaving many centers with insufficient staff to care for residents,” said Mark Parkinson, president, and CEO of the American Health Care Association and National Center for Assisted Living, which represents over 14,000 nursing homes. “It will exacerbate an already tough labor shortage.” This move will have the reverse impact of what was intended, and it will jeopardize our capacity to offer quality care to our residents.”
Nationally, immunization rates for nursing home staff members are significantly lower than those for residents. According to the American Association of Retired Persons, 78 percent of residents at long-term care facilities are completely vaccinated — while just 56.7 percent of staff members are.
Liistro told that his staff continues to voice reservations about the vaccine’s safety and efficacy, despite the fact that nursing home cases and fatalities have decreased significantly since nursing homes were prioritized for vaccination.
“We have around 125 individuals who are not vaccinated,” Liistro remarked of his workers. “My estimate is that 80% will receive vaccinations, 10% will receive exemptions, and the remaining 10% will leave.”
“However,” he said, “I am certain that we will find people who want to work in a safe atmosphere with ethical companies.”
Managers at John Knox Village, a 430-bed independent nursing facility in a Kansas City suburb, say they are seeing competition from outside the health care sector. Along with losing nurses and certified nursing assistants to other nursing homes and hospitals that pay more, the institution recently lost its long-time maid to a warehouse job that paid an extra $3 an hour.
According to John Knox Village spokesperson Emily Banyas, the facility increased salaries for certified nursing aides to between $11 and $12 an hour last year in order to remain competitive with retailers such as Target and Walmart. However, the big-box shops have increased their pay and introduced advantages such as college tuition and relocation fees.
“It’s becoming a catastrophe for senior living homes,” Banyas explained.
The majority of Florida’s 310 nursing homes and 23 assisted living facilities surveyed by the Florida Health Care Association last month reported staffing shortages.
As a result, many Florida institutions, according to FHCA spokesperson Kristen Knapp, are forced to hire temporary staffing firms to replace vacancies. This has resulted in an additional $22.7 million in costs for facilities in the state, according to the Agency for Health Care Administration.
Additionally, Knapp stated that some institutions have been unable to accept new patients due to a staffing shortage.
The long-term care labor issue in Pennsylvania has “outgrown control,” according to Zach Shamberg, president and CEO of the Pennsylvania Health Care Association.
As with Florida, providers in Pennsylvania have depended primarily on agency personnel or contractors to satisfy staffing demands — but even those agencies are now suffering a manpower crisis.
“Other industries, such as hospitals, have the financial resources to provide lavish incentives and swiftly increase wages,” Shamberg explained. “Long-term care providers just cannot keep up, which results in people departing for other health care and non-healthcare professions.”
Dr. David Gifford, the AHCA/chief NCAL’s medical officer, stated that a long-term solution is critical.
“Nursing homes are constantly competing for personnel,” Gifford explained. “Many providers struggle to recruit and retain caregivers, who may frequently find less demanding work in other settings, such as hospitals or sectors with higher compensation.”
“This has been a continuous and critical issue for long-term care, which the COVID-19 epidemic has aggravated,” Gifford added. “The final consequence will be seen by our nation’s elders, who may suffer a lack of long-term care options.”